Phalanges Definition
The type of bones which form the skeleton of digits i.e. the fingers and toes of the body are primarily known as phalanges bones. The human body has a total of fifty-six phalanges, with three phalanges for each finger and toes except for two phalanges per thumb and large toes in feet. The phalanges are normally linked with each other at hinge-like inter-phalangeal joints which is for extension purpose. In many cases, the phalange bones are fused with each other.
Phalanges Location and Structure
Normally, the width of the phalange bones are extensively smaller than their usual length, given their structure is designed to support long digits of the human body. The standard digital formula of a phalange is said to be 2+3+3+3+3 based upon the number of bones for each digit starting from the thumb or large toes towards the smallest finger or toes. The phalanges of legs are longer than those of hands due to their comparatively large size. The specified digit bones for hands are named based on their locations, i.e. proximal, intermediate and distal with respect to their distance from the main phalange bone connecting to the forearm and tibia. The main connective phalanges for hands are referred to as metacarpals while for the foot is termed as metatarsals. The metacarpals and metatarsals are attached together through ligaments at the metacarpophalangeal and metatarsophalangeal joints. Further, these phalanges are connected with muscles of the palm, forearm, foot muscles by tendons starting from the base of the skeleton.
Types of Phalanges
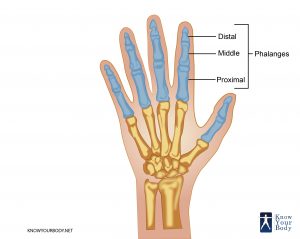
- Proximal Phalanges
These are the primary phalangeal bones which connect the digit forming structure to the limb bones. The shape of proximal phalanges in humans are observed to be broad with a concave surface near the palm. It connects the base of the limb with the metacarpophalangeal joint to facilitate movement around the writs and ankles.
- Intermediate Phalanges
As the name suggests, these types of phalanges are intermediate in location and size as compared to other bones of phalanges. Also, these are not present in every digit. For instance, intermediate phalanges are always observed to be missing from thumbs and large toes and hence their digital formula is said to be 2. Their location is mainly in between the proximal and distal phalanges which explains it to be connected with two interphalangeal joints.
- Distal Phalanges
These are the farthest phalanges from the limbs and are commonly called as the terminal phalanges. These are the most diverse phalangeal bones as it serves a number of purposes including supporting the fingertips with cushion flesh under the fingers and toes. These cushion flesh of fingertips have a number of nerve endings for sensitivity and are said to have gone under numerous evolutionary adaptations for a fine motor coordination with the brain. These phalanges also have minor extensions which are small and flat and are called apical tufts and support nails of the digits for a better protection and attacks on preys.
Phalanges Function
The phalanges support the basic framework of the digits by forming a closely linked structure for smooth motor function and digit precision. Majority of voluntary living functions are performed by digits which in turn are flexible due to the structure of phalanges the way they are – be it tool making, grasping things, or crafting things to facilitate human loving in the long run. These are considered to be the ‘executors’ of the task that our brain directs them to. This is exactly the reason why they are considered to be of prime importance for evolutionary process of hominids.
Phalanges Origin
Since the phalanges are an integral part of our skeleton system, these are present inside the body with the mesodermal origin and are mostly living in nature. An infant human has around three hundred and five bones which are reduced to just two hundred and six by adulthood due to linking and attachments formed during growth, out of which phalanges are never connected after birth so they do not reduce in numbers.
Phalanges Clinical Significance
Usual accidents or traumas can cause clinical fractures which can cause temporary to permanent impairment in these areas. The common injuries to proximal phalanges range from fractures related to connecting limbs or dislocation of connecting joints. They are most commonly treated with plaster of Paris bandages for stability and recovery of the original condition of the bone structures and links and are also treated with screw insertions wherever necessary. The usual screw Insertion surgeries include the usage of anesthetics and analgesics to reduce pain in the injured area. The area is usually suspended to immobilization till the original alignment of the said bone is not fully recovered.
Phalanges FAQs
What do we do in case of pain in fingers or toes? Is it a sign of phalangeal injury?
Not all the pains in the fingers and toe areas are a result of phalangeal injury but ignoring them can be fatal for your locomotion and movement. They can also be a resit of muscle injury but the pain can cause inflammation your tendons which in turn connects to your phalanges, so an appointment with an orthopedic surgeon would be the best option to medically recover from the pain.
What are the usual medical tests to screen any possible injuries for my phalanges?
An injury to your phalanges can be fatal and can possibly leave you immobilized permanently. It is best to visit an orthopedic surgeon to get yourself diagnosed and treated if you face an injury. They usually prescribe a screening test from a range of X-Ray to MRI (Magnetic Resonance Imaging) depending upon the type of your injury. Generally, people find it scary to undergo these screening tests due to the fear of exposure of oncogenic X-Rays but once in a whole exposure to these rays doesn’t really cause a harm. Besides, they are important to get your diagnosed.
What is the recovery time period in case of a phalangeal fracture?
A fracture can be of numerous types ranging from a hairline fracture to a dislocation or a complete breakage of a single phalangeal digit based upon your accidental injury to the digital skeleton. Based on the level of injury, your orthopedic surgeon will immobilize your injured area with a plaster of paris base bandage and will tell you about the possible recovery period. This can range from a couple of weeks to a couple of months totally dependent on your injury and recovery capability of your body. But we assure that you don’t have a reason to worry at all.

No comments yet.